Before delving into plantar fasciitis and heel spurs, it is important to have read and understood three previous posts, We Are Just a bunch of moving parts, The Core and The Hinge. The premise is that foot pain and deformity develops due to the breakdown of normal, developmental movement patterns we first learned, when we learned how to walk. These articles lay the groundwork for truly understanding the Granddaddy of misunderstood and mistreated conditions: Plantar Fasciitis.
What is the Plantar Fascia?
Fascia is a soft tissue of the body that, under a
microscope, is of almost the same composition as ligaments and tendons. The major differences are in regards to
function. Each of these structures
(tendon, ligament, and fascia) starts from bone. Tendons attach muscles to bones, and cross
joints that they either intend to move or stabilize. As I like to think of it, tendons exert the Will
of the muscle at a given joint.
Ligaments attach bone to bone at a joint, and only serve to help
stabilize that particular joint. Fascia
has a more indirect role. It has one
solid attachment on bone, and then fans out across a broad area inserting into
joints, skin, and other soft tissue structures at a distance from its
origin. The role of fascia is a
secondary stabilizing role. It more or
less ties things together. It doesn’t
assist movement in the way that tendons do.
In fact, if anything, it helps resist movement by acting as a tension
band; something that will tense to a point and then stop (key point!). It lacks the direct strength of ligaments by
being typically larger and less defined in its purpose and it lacks elasticity,
so it won’t stretch (another key point!).
The key areas of fascia in the body are the bottom, or Plantar surface
of the feet, the side of the upper leg/quads (Ilio Tibial band), low back
(thoracolumbar) and back of the neck (nuchal fascia).
What are heel spurs?
Spurs are projections of bone that develop at the attachment
sites of tendons, ligaments, or fascia.
The attachment of soft tissue to bone is very strong. On a cellular level, there is an intertwining
of bone cells and the cells of either the tendons, ligaments, or fascia that
allows those structures to literally become the bone, not just attach to the
bone. When there is too much tension at
the attachment sites, the bone cells will build in response to that tension,
and specifically, build INTO the tendon, ligament, or fascia. On an x-ray, bone is most visible, and this
well-defined projection of bone into the soft tissue structure will become
visible. X-rays are 2 dimensional
images, and therefore, the projection of bone in certain views will appear
spur-like. With some exceptions, it is
NOT typical for people to feel the spurs.
Despite this, plantar fasciitis is often called Heel Spur syndrome due
to the typical presence of heel spurs on x-rays of patients who experience
plantar fasciitis. However, spurs are
not present in everyone who has plantar fasciitis, just as they are present in
many without plantar fasciitis. Spurs
are not caused by pain, they are caused by excess tension. Excess tension does not always lead to
symptoms, yet over time, it will almost always lead to the appearance of
spurring on X-rays.
What is Plantar Fasciitis?
Plantar fasciitis is literally defined as inflammation of
the plantar fascia. Beyond this point,
many assumptions are made about what it is, what causes it, and how to treat
it. Let’s start by defining what plantar
fasciitis is NOT. It is NOT an injury to
the fascia. It is NOT an overuse injury. It is NOT because of a heel spur, a lack of
arch support, or being too heavy.
Plantar fasciitis IS something that is felt; a symptom. When the tension placed through the fascia is
greater than what it can handle physiologically, it will become inflamed. If the tension is not reduced in some way,
then symptoms often follow. The problem
I have with how Plantar Fasciitis is usually defined and treated, is that the
symptoms people experience are treated as the problem. The symptoms however are only where the
underlying problem is manifesting itself.
The real key to understanding plantar fasciitis, is to understand that
it is a chronic movement disorder which involves the entire body. A movement disorder that forces too much
tension through the fascia. If it were
truly an injury, then rest would heal it, and being on it would hurt. Most people with plantar fasciitis are OK
with certain activities and only hurt after activity, or more specifically,
after periods of rest following activity as well as the first few steps in the
morning. Of course, left unattended, symptoms may, and
often do, progress to a more chronic state where pain is experienced throughout
the day in varying degrees.
Mechanics of Plantar Fasciitis:
Concept:
As we’ve learned in the prior articles, proper mechanics (proper movement) is dependent on the harmony that exists with the movements our body’s make. It either works flawlessly, or it doesn’t. Most people who are reading this and old enough to follow along should understand this. Due to many years of being forced to sit in chairs as school kids and being forced to wear shoes that constrain our feet, our adult movement has no choice but to be flawed. Therefore, we will not be using all of our joints in the most efficient and effective manner possible. In the previous article about the ankle, The Hinge, I explained what happens when the ankle doesn’t function properly. As forward movement occurs, and the ankle doesn’t do its job and bend, the bending forces are going to be taken up by other joints in the middle of the foot. The plantar fascia, connecting the heel to the ball of the foot, is then placed under strain beyond what was intended.Technical description:
As the foot hits the ground, it usually does so striking the
heel first. Due to the improper
functioning of our body mechanics (see prior posts), our heels typically land in front of our bodies center line
of posture. As we continue to move our
body forward, the midfoot, and then forefoot (ball of foot just behind the
toes) load onto the ground as weight transfers from heel to toe. Once the foot is fully loaded, it’s time for
the body to pass over that foot. In
normal situations, the ankle is able to bend (flex) over a stable foot and
forward movement occurs without compensation in the foot. When the ankle does not bend as it should
despite the forward movement of the body, the middle of the foot bends
instead. This will force the heel off
the ground while the front of the foot is pinned against the ground. As forward motion continues, there is
increased strain applied through the single bony attachment site of the plantar
fascia, which is under the heel. Depending on factors of body type,
compensation patterns elsewhere, gait patterns, shoe selection and activity,
pain may be felt in one of several places.
The most common is just in front of the heel on the inside. This corresponds to the main attachment site
of the plantar fascia and where the strain is maximized. Pain can also be felt in the middle of the fascia,
also on the inside part of the foot, but more under the arch. This is another high area of strain, but off
the attachment site. Lastly, pain can be
felt on the back of the heel at the insertion site of the Achilles tendon. Though this diagnosis would be consistent
with Achilles tendonitis, the mechanism of pain is virtually identical to that
of plantar fasciitis, just with a different set of underlying factors that
results in a different area of pain.
The changes that would be seen on an x-ray are as follows
(Figure 1):
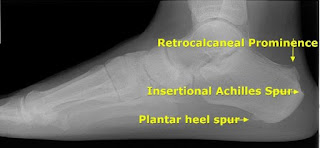
Figure 1: Plantar Heel Spur, Insertional Achilles spur,
Rectrocalcaneal Prominence
- A spur of bone at the plantar fascia origin site as seen on one of the x-ray views. This is not a single point of bone, but rather, a shelf of bone along the entire attachment site. But when viewed on a 2 dimensional image, it appears as a spur.
- The spur may also be seen on the Achilles attachment site in the back of the heel. This may be the only finding in cases of plantar fasciitis. Again, spurs on the heel are NOT indicators of pain or symptoms. They represent chronic tension over time at the attachment sites of tendons or fascia. With plantar fasciitis or Achilles tendonitis, there is an underlying, chronic high tension at the attachments sites that often leads to the appearance of spurs on bone regardless of symptomatology.
- Enlargement of bone on the top and back of the heel bone/calcaneus. This is termed a retrocalcaneal prominence. It occurs over time when the ankle doesn’t bend as it should and the pull of the Achilles on the back of the heel is higher than it should be. Through a process known as “Wolf’s law,” bone builds up when placed under increased stress.
What else can cause Heel pain if it’s not Plantar Fasciitis?
Just about everyone who comes to me with Heel pain thinks
they either have “heel spurs” or “Plantar” as it is so often referred to. Plantar fasciitis, as has been described, is
a symptom due to high strain through a structure (fascia) that can only take so
much.
- Achilles Tendonitis
- Growth plate inflammation in children (Sever's disease)
- Tight heel cord (Equinus)
- Stress fracture of the Calcaneus (heel bone)
- Bursitis under or behind heel
- Nerve irritation from the sensory nerves that innervate the bottom of the heel. This can be felt directly under the heel, but there is a trigger elsewhere causing pain to refer under the heel
- Infection (more common in children with open growth plates, though still uncommon)
- Decreased fat padding
- Irregular bone spurring (outside the fascia)
- Plantar fascia tear
- Bone infections (hematologous osteomyelitis in children with open growth plates)
- Systemic Arthritis (Reiter's disease for example)
- Congenital deformities to heel
- DVT (blood clots in calves) and circulatory problems that could be far more serious
Often times, when one of these other causes of heel pain is
present, then plantar fasciitis will ALSO be experienced. The reason for this is simply that when the
body is experiencing pain, movement will be guarded. When movement becomes guarded, then the
tension and stress placed through the fascia increases and symptoms can result. The typical symptoms being pain with the
first few steps out of bed in the morning or standing after periods of rest
(post static). One of the key
distinctions between plantar fasciitis and one of these other causes is this;
plantar fasciitis typically doesn’t hurt with activity! It certainly can when it becomes more
chronic, but the most significant symptomatic period is post-static (standing
after a period of rest) and again after activity or finally at the end of the
day, as opposed to times when you are active.
So if you are experiencing pain with activity as well, then it often
indicates one of these other processes is occurring as well.
Why doesn’t it hurt all the time?
As previously mentioned, plantar fasciitis typically is not
an injury. It’s something that is felt
due to tension and load being forced through a tissue that is unable to hold
up. Once moving, it usually takes a few
steps or a few minutes for the body to be able transfer the tension
elsewhere. Once that occurs, then the
fascia is “protected” by the tension shift and the symptoms will be reduced or
disappear altogether. If it is an
injury, then the fascia, or any injured part for that matter, would feel
symptoms with even very little stress placed through the tissue. Therefore, if it does hurt at all times when
standing or walking on the foot, then there would also happen to be an injury
to the fascia, or some other process more significant than plantar fasciitis.
What to Do?
I always feel that this is a loaded question; what to do
about what, symptoms or underlying problems?
Therefore, I think it’s important to take a segmental approach. 1st, treat the symptoms. 2nd, address the immediate factors
that relate to the symptoms. Lastly,
identify, and help the patient understand where the problems are ultimately
originating, and offer them the choice of pursuing fundamental changes that can
lead to long term success. In short,
there are short term goals and long term goals.
If you do a google search, as most do, about how to treat
plantar fasciitis, you will come up with many helpful ways to deal with plantar
fasciitis and even “cure” it. Icing,
including rolling the arch on a frozen water bottle, has always been one of the
easiest and best methods of home remedies.
Ibuprofen and other anti-inflammatory medications can work wonders at
times. Stretching the calves and bottom
of the foot, be it by hanging off a step, wearing a splint that you sleep with
at night (night splint) or other variation can also be helpful for many
people. Resting the painful foot by
avoiding activity often goes without saying and many people even go so far as
to elevate the foot every chance they can.
Buying new shoes or arch supports is often one of the first knee jerk
reactions to foot pain and can be effective in the short term. After all, your friend who had plantar
fasciitis once told you it worked for him, so it will definitely work for you!
While these remedies are all safe and actually quite helpful, they really don’t
begin to get at the root of the problem as this article has set out to explain. Bottom line, if you’re going to self-treat,
be sure that whatever you are doing is helping and the pain is not getting
worse as a more serious condition is possible.
What I believe are the safest of home remedies, are the ones
in which you are helping both the symptoms and the factors leading to the
symptoms. I typically suggest some type
of anti-inflammatory action, be it from ibuprofen in those who can take the
medication safely, to icing several times a day, especially before bed. Should ice actually irritate the condition,
then your thoughts should head away from plantar fasciitis and possibly to some
form of nerve irritation. “Stretching”
can be very helpful. However, the goal
of stretching is what you are after, not the ACT of stretching. Please review my article Is Stretching Good For You? to understand what I’m looking for in terms of the
goals of stretching. The real goal is to
relax the muscles in the calves that all attach to the foot. The more relaxed they are, the better they
can do their job in helping support and control the movements in the foot. I use the Triggerpoint Performance Therapy tools in my office to help patients help themselves. Compression socks are also a wonderful tool
to help with muscle recovery, staying with the theme of helping the muscles
function optimally and do the job they are designed to do. Avoiding activities that make you worse is
crucial until symptoms subside. If being
active isn’t making the foot any worse, but not helping the situation, and
you’ve done the above, then perhaps it’s time to understand more about your
condition and take treatment to the next level.
In our office we really try and understand why the pain
developed. We will do whatever is
necessary to help get people out of pain, keep them active and keep them from
developing recurring pain in their feet as well as hopefully identifying and
helping them to fix underlying problems in their body before the pain turns to
the knees, hips, back and neck. I really
do look at every episode of heel pain (foot pain really) as an opportunity to
understand some of the flaws in how we use our bodies and as an opportunity for
the patient to help “right the ship” before it’s too late. The following is a list of things that are
often recommended and why and when they may be helpful:
Cortisone injections:
These are anti-inflammatory medications.
Think of it like crushing up aspirin and putting it right at the source
of pain. Not all cortisone is created
equal. I use a very fast acting steroid
that will be out of the body in a day.
It is important for people to not guard against pain and that’s why it’s
important to treat symptoms. Cortisone
often gives people a chance to start helping themselves more effectively. Cortisone is not the cure. It can also be used safely despite the
concern many people have.
Night Splints:
These can be helpful for people whose pain is significant with the first
few steps out of bed. It should be
effective within the first week and if after 7-10 days there hasn’t been
change, then it’s not going to be helpful.
Often, I’ll have patients start with the Triggerpoint tools before
getting out of bed as night splints can negatively affect ones sleep, and the
use of the massage tools before getting out of bed will have the same result.
Orthotics:
These are NOT arch supports. The
goal of an orthotic is to stabilize the foot.
This is done through controlling the position of the heel relative to
the position of the leg. I will have to
write an entire article devoted to orthotics to properly explain them, but
here’s an analogy that is fairly spot on;
An off the shelf arch support (Dr. Scholls, Goodfeet, Powerstep, Spenco,
etc) are like reading glasses. Sometimes
people just need magnification to see better with reading, and some people just
need a little pressure in their arches to feel better. Orthotics are like Prescription eyeglasses
when someone needs their poor vision corrected. Finally, some people choose to have Lasik
surgery to definitively correct their vision, just as some doctor’s may suggest
surgery to remove the heel spur or release the tight fascia to help with heel
pain.
Surgery:
Surgery
is often a last resort in most elective situations, though not always depending
on the condition. With heel pain
however, I look at surgery as absolutely the last resort, especially considering
the fact that I don’t believe the main problem involves the fascia, but
elsewhere. That said, if a patient has
tried everything and still no relief, there are several procedures that I
perform and have had success over the years.
The first is an EPF (endoscopic plantar fasciotomy). In this procedure, 2 tiny incisions are made
on each side of the heel and a fluted tube is placed from one side to the
other. A camera is inserted, and while
visualizing the plantar fascia, a small blade is used to release the tight
portion of the plantar fascia. The key
to this procedure, and any surgical procedure releasing the fascia, is post-operative
casting for 4 weeks to allow the fascia to heal in a lengthened position. The second procedure performed is a more
traditional approach with an open incision on the inside of the heel, surgical
release of the plantar fascia and resection of the spur of bone from the bottom
of the heel. There are several
variations on a theme to these procedures, but the essence remains the same;
release the plantar fascia so that it’s not too tight.
Alternative Procedures:
PRP
(platelet rich plasma) can be used to help the fascia heel from within. Blood is drawn from the patient and then a
centrifuge is used to “spin” out the platelets from one’s own blood. Platelets contain the growth factors
necessary to heal damage within our body of any tissue type. Here, a high concentration of platelets is
injected into areas of pain. Topaz (radiofrequency therapy) is
another modality that helps the tissue heal from within. A radiofrequency probe is inserted into the
fascia every 5 mm over the areas of pain and the energy released in the fascia
is geared towards allowing new circulation to develop within the fascia as the
injuries made in the process attempt to heal themselves. ESWT
(Extra corporeal Shock Wave Therapy) uses sound waves to bombard the spur of
bone and the fascia in an effort to create an acute injury that the body needs
to heal. With any of these, and any
newer therapy on the market (Prolotherapy included), one has to realize that it
is the Symptoms being treated and not the problems that caused the
symptoms. While these all can, and often
do, provide symptomatic relief, they also enable people to neglect real
problems of movement that can and most often do lead to problems in other parts
of the body down the road of life.


No comments:
Post a Comment
Note: Only a member of this blog may post a comment.